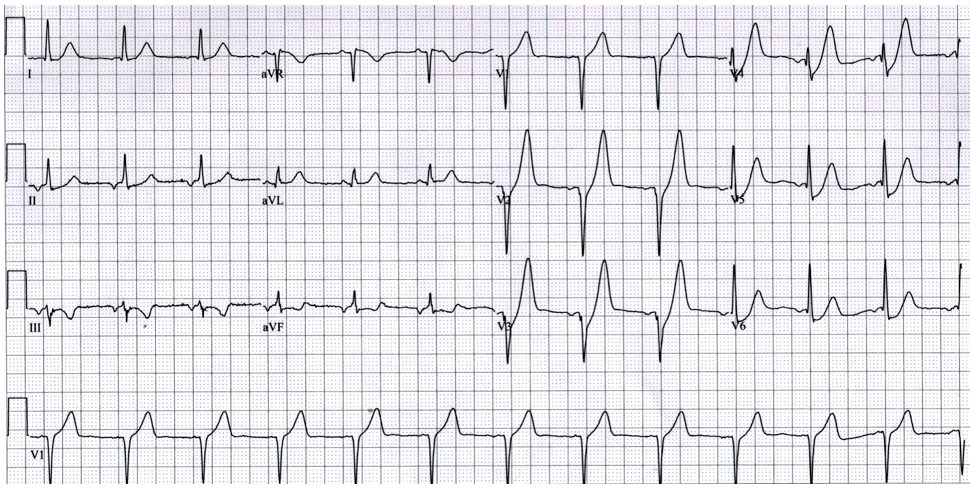
Eventually, the heart may fail to pump with as. The thickened heart wall loses elasticity, leading to increased pressure to allow the heart to fill its pumping chamber to send blood to the rest of the body. The delay or blockage can occur on the pathway that sends electrical impulses either to the left. Left ventricular hypertrophy is enlargement and thickening (hypertrophy) of the walls of your hearts main pumping chamber (left ventricle). It sometimes makes it harder for the heart to pump blood to the rest of the body.
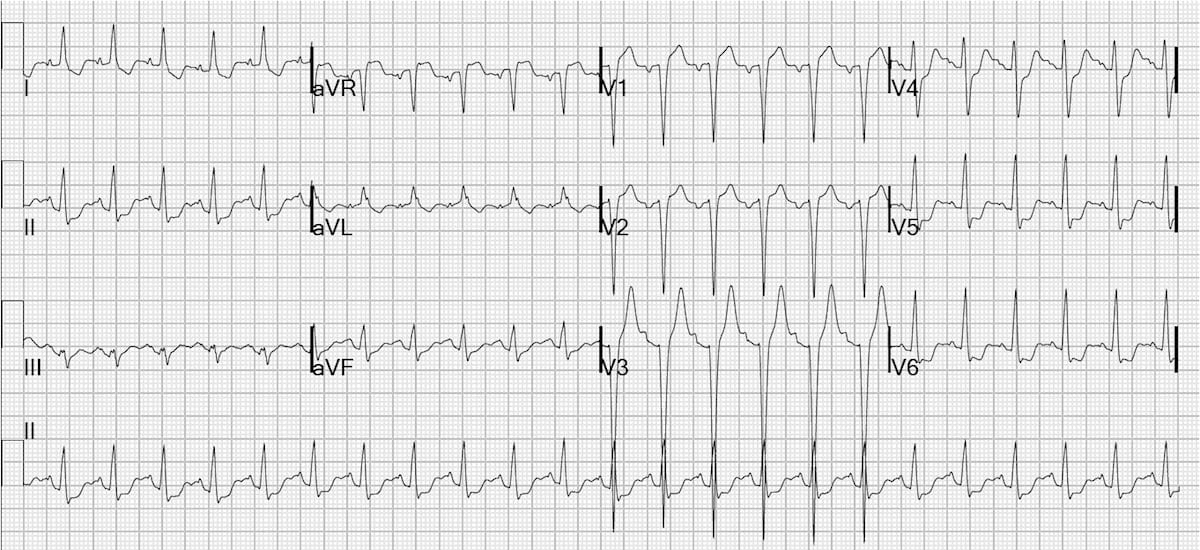
Many times when the patient presents with an acute MI, they are taken to the cardiac catheterization lab. lar conduction delay IVCD + LVH and even STEMI on top of ST segment. NonST-elevation acute coronary syndromes: AHA/ACC: 2014 S1.4-20 Assessment of cardiovascular risk: ACC/AHA: 2013 S1.4-21 ST-elevation myocardial infarction: ACCF/AHA : 2013 S1.4-22 Acute myocardial infarction in patients presenting with ST-segment elevation: ESC: 2012 S1.4-23 Device-based therapies for cardiac rhythm abnormalities: ACCF/AHA/HRS: 2012 S1. The frequency of repolarization changes were associated with the presence of CHD in the women and with the magnitude of BP elevation, the degree of a cardiovascular risk, the grade of HD, and the presence of both echocardiographic and electrocardiographic signs of LVH. I had a pre-op ECG with abnormal results citing nonspecific ST abnormality and a normal sinus rhythm. Bundle branch block is a condition in which theres a delay or blockage along the pathway that electrical impulses travel to make the heart beat. Heart block associated with an inferior wall MI is usually proximal to the His-bundle and transient, whereas AV block secondary to an anterior wall MI is more distal to the His-bundle and often persists. Now, when the EKG shows inappropriate concordance (J-point and ST-segment elevation in positive leads, and J-point and ST-segment depression in negative leads), there is a 90 likelihood that the. myocardial infarction from ST elevation secondary to nonischemic etiologies. The classical tension syndrome and nonspecific repolarization changes were observed in 7 and 26% of cases, respectively no significant differences were found in their detection rates between the males and females. The electrocardiograms of 234 patients with AH (104 males and 130 females) were analyzed, by taking into account the magnitude of blood pressure (BP) elevation, the degree of an overall cardiovascular risk, the grade of hypertensive disease (HD), the presence of coronary heart disease (CHD), as well as echocardiographic and electrocardiographic voltage criteria for left ventricular hypertrophy (LVH). It can be the first ECG manifestation of an evolving myocardial infarction and it represents the ECG criteria for thrombolytic therapy. To estimate the detection rate of tension syndrome and nonspecific repolarization changes in patients with arterial hypertension (AH). Acute or dynamic ST elevation can be due to severe transmural ischemia secondary to thrombus, spasm or a tight fixed coronary artery lesion or a combination of these situations.
